| Journal of Hematology, ISSN 1927-1212 print, 1927-1220 online, Open Access |
| Article copyright, the authors; Journal compilation copyright, J Hematol and Elmer Press Inc |
| Journal website http://www.thejh.org |
Case Report
Volume 1, Number 1, February 2012, pages 28-31
An Unusual Cause of Iron Deficiency Anemia in a Child With Colonic Lithobezoar: Case Report and Review of the Literature
Nergis Onera, Zuhre Kayaa, c, Zafer Turkyilmazb, Ramazan Karabulutb
aThe Pediatric Hematology Unit of the Department of Pediatrics, Gazi University Faculty of Medicine, Ankara, Turkey
bDepartment of Pediatric Surgery, Gazi University Faculty of Medicine, Ankara, Turkey
cCorresponding author: Zuhre Kaya, Gazi University Medical Faculty, Besevler, Ankara, 06500, Turkey
Manuscript accepted for publication February 16, 2012
Short title: Cause of Iron Deficiency Anemia
doi: https://doi.org/10.4021/jh105e
| Abstract | ▴Top |
Along with literature search, we aimed to emphasize the importance of psychiatric evaluation, existence of pica history as the reason for iron deficiency anemia, and the timing of early surgical intervention to prevent development of intestinal obstruction in a 14-year-old boy diagnosed for colonic lithobezoar.
Keywords: Iron deficiency anemia; Lithobezoar; Child
| Introduction | ▴Top |
Bezoar is a cluster of mass forming as a result of ingestion of food or foreign materials that cannot be absorbed by the intestinal system [1, 2]. Lithobezoar occurs by ingestion of stones and is a very rare cause of intestinal obstruction in childhood. Signs and symptoms range from mild to severe according to the anatomical region of the stone accumulation [3-11]. If there is iron deficiency anemia (IDA) concomitantly, pica should definitely be questioned in the history [8, 11].
We report the predisposing factors, clinical presentation, diagnostic evaluation and therapeutic management of one case with colonic lithobezoar in the light of literature.
| Case Report | ▴Top |
A 14-year-old boy presented with the complaints of pallor, abdominal pain and constipation recurring intermittently for two years. He had been admitted several times to other hospitals for IDA requiring iron treatment. At presentation, he was pale and anxious. There were decreased in bowel sounds and tenderness in lower abdominal quadrants on physical examination, and a solid mass on rectal examination. Plain abdominal radiography showed an image of disseminated opacity in the region corresponding to descending and sigmoid colons (Fig. 1). Laboratory findings were as follows: hemoglobin, 5.5 gr/dl; hematocrit, 19%; mean corpuscular volume, 51 fl; mean corpuscular hemoglobin, 15 pg; mean corpuscular hemoglobin concentration, 28.9 g/dl; red cell distribution width, 28.9%; platelet count, 608,000/mm3; white blood cell count, 14,200/mm3; serum iron, 6 µg/dl; iron-binding capacity, 372 µg/dl; reticulocytes, 1.04%; and serum ferritin, 1 mg/dl. Peripheral blood smear showed hypochromic, microcytic erythrocytes. There was also pica history.
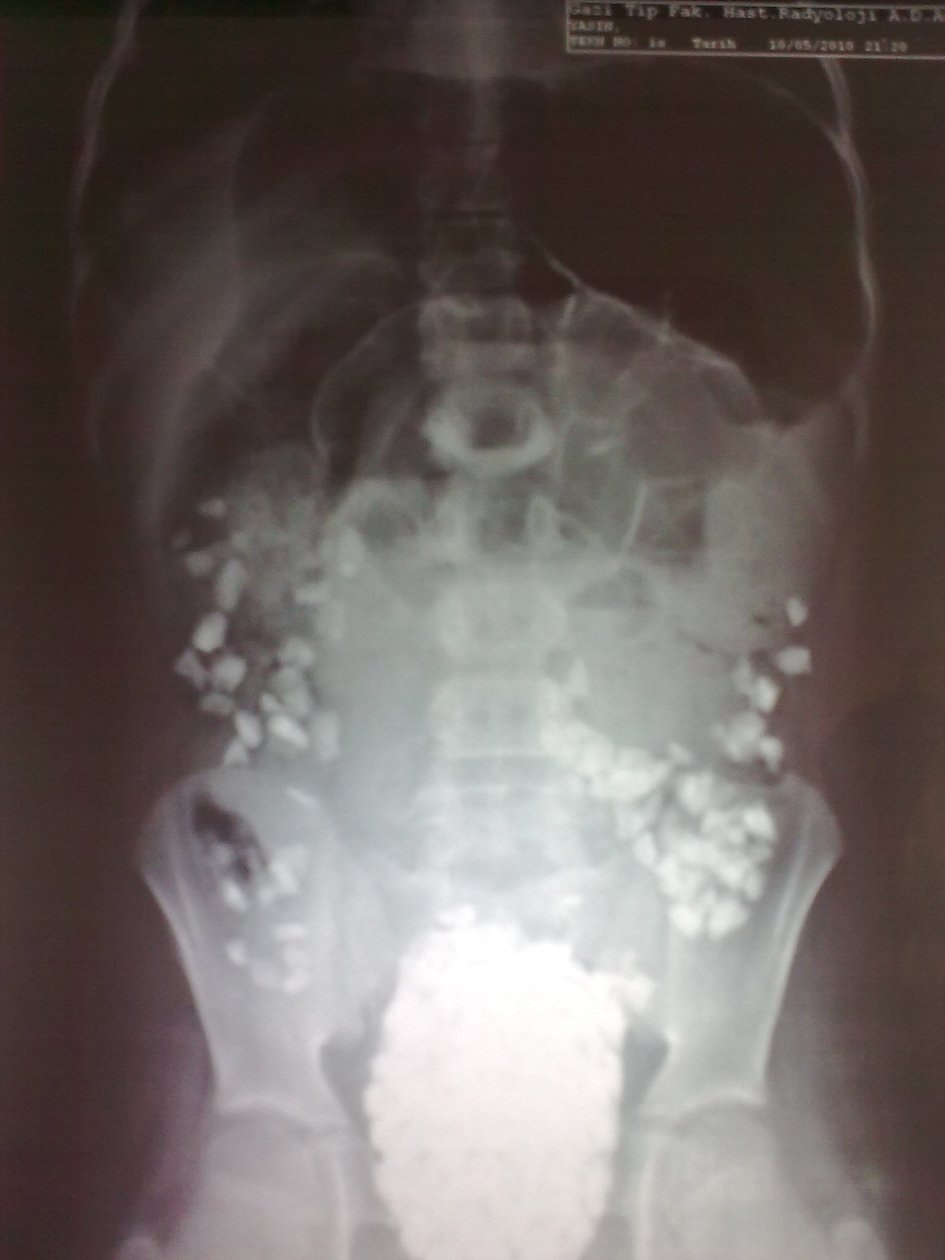 Click for large image | Figure 1. Plain abdominal radiography showed an image of disseminated opacity in the region corresponding to descending and sigmoid colons. |
Before surgical procedure, packed red cell transfusion was administered to the patient. Anal canal was dilated via forceps under general anesthesia and one kilogram of pebbles was removed out of the sigmoid colon. The patient was assessed as normal by the Department of Pediatric Psychiatry. As to the familial and socioeconomic background, he was poor and lived in a crowded and stressful house and his school performance and family relationship was awful. The patient, whose anemia improved, was discharged after starting iron treatment. He could not be reached by his contact information, and it was realized that he was lost to follow-up.
| Discussion | ▴Top |
Bezoars are concretions of undigested foreign material, which may occur anywhere in the gastrointestinal tract, usually in the stomach [1]. Trichobezoar or human hairball is the most common type of bezoar in humans, whereas lithobezoar, which is stone accumulation in the intestinal system, is very rare [2]. We searched PubMed to identify the reports on colonic lithobezoar in literature using the keywords “colonic lithobezoar” or “rectosigmoid bezoar” and only seven cases have been previously reported from developing countries such as India, Turkey and Nigeria [3-7, 9, 10]. Other similar case reports in Turkish literature, not indexed in PubMed, were also added into the case list [8, 11]. Among those nine cases, six were male and three were female. Although trichobezoar is more common in girls and adolescents, lithobezoar is reported mostly in boys as in our case and literature search (Table 1) [2].
 Click to view | Table 1. Summary of the Demographic and Clinical Characteristics of the Cases With Colonic Lithobezoar |
Most of the lesions are clinically silent and found incidentally during plain abdominal radiography and rectal examination for constipation or abdominal pain as in our case. The clinical manifestation depends on the location, size and direction of the stone accumulation. Although rectal examination is a simple and inexpensive way to diagnose a bezoar, abdominal radiography offers an immediate diagnosis, if the bezoar is visualized. An image of disseminated opacity in the abdominal radiography is important in the diagnosis of colonic lithobezoar. Bezoar had a characteristic appearance in abdominal radiography in each nine cases [3-11]. When the bezoar is in the colon, intestinal obstruction has been reported and in some cases, they can lead to life threatening complications [3, 7, 8].
Underlying psychiatric problems and mental retardation should definitely be investigated in such cases. Although no mental retardation or psychiatric problems were detected in the present case, there are three cases reported in the literature [4, 7, 11]. In children, bezoars are associated with pica, mental retardation, and coexistent psychiatric disorders. Eating disorders are psychiatric disorders presenting various problems in eating behavior and have biological, psychological, social, and familial factors as important causes [12]. It is possible that ingestion of stones started because of his stressful life events and familial conflict, but eventually resulted in real intestinal pathology in our case. After removing the stones and starting iron deficiency treatment, the patient could be reached no more. Therefore, there is no clear estimation on recurrence of the condition.
If there is IDA in the patient with colonic lithobezoar, pica should definitely be questioned in the history. Although pica is a common condition in children, and mostly improves spontaneously, if continues, IDA may develop. In the literature, there were eight cases reported with association of colonic lithobezoar and pica [3, 5-11], however, there were two cases with mild pallor, one case with hematochezia and, only two cases that developed IDA [3, 5, 8, 10, 11].
In conclusion, the presented case suggests that although IDA has a multifactorial etiology, subtle history of pica and concomitant bezoar should be taken into consideration as a possible additional factor in severe or persistent IDA. Clinicians should also be aware of colonic lithobezoars signs and symptoms in order to prevent the occurrence of intestinal obstruction in such cases.
| References | ▴Top |
- Andrus CH, Ponsky JL. Bezoars: classification, pathophysiology, and treatment. Am J Gastroenterol. 1988;83(5):476-478.
pubmed - Gonuguntla V, Joshi DD. Rapunzel syndrome: a comprehensive review of an unusual case of trichobezoar. Clin Med Res. 2009;7(3):99-102.
pubmed doi - Rathi P, Rathi V. Colonic lithobezoar. Indian J Gastroenterol. 1999;18(2):89.
pubmed - Ratan SK, Grover SB. Giant rectosigmoid stone bezoar in a child. Clin Pediatr (Phila). 2000;39(8):500-502.
pubmed doi - Vijayambika K. Lithobezoar. Indian Pediatr. 2004;41(11):1168.
pubmed - Tokar B, Ozkan R, Ozel A, Koku N. Giant rectosigmoid lithobezoar in child: four significant clues obtained from history, abdominal palpation, rectal examination and plain abdominal X-ray. Eur J Radiol Extra. 2004; 49(1):23-24.
- Narayanan SK, Akbar Sherif VS, Babu PR, Nandakumar TK. Intestinal obstruction secondary to a colonic lithobezoar. J Pediatr Surg. 2008;43(7):e9-10.
pubmed doi - Numanoglu KV, Tatli D. A rare cause of partial intestinal obstruction in a child: colonic lithobezoar. Emerg Med J. 2008;25(5):312-313.
pubmed doi - Sheikh MS, Hilal RM, Misbha AM, Farooq AR. Colorectal lithobezoar: A rare case report. J Indian Assoc Pediatr Surg. 2010;15(2):62-63.
pubmed doi - Mohammad MA. Rectosigmoid lithobezoar in a eight-year-old. Afr J Paediatr Surg. 2010;7(1):38-39.
pubmed - Torun YA, Torun E, Ergul AB, Karakukcu M, Patiroglu T. A rare cause of iron deficiency anemia in a child: Lithobezoar. Turk J Haematol. 2011; 28(3):252-253.
- McEwen C, Flouri E. Fathers' parenting, adverse life events, and adolescents' emotional and eating disorder symptoms: the role of emotion regulation. Eur Child Adolesc Psychiatry. 2009;18(4):206-216.
pubmed doi
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Journal of Hematology is published by Elmer Press Inc.


