| Journal of Hematology, ISSN 1927-1212 print, 1927-1220 online, Open Access |
| Article copyright, the authors; Journal compilation copyright, J Hematol and Elmer Press Inc |
| Journal website http://www.thejh.org |
Case Report
Volume 3, Number 4, December 2014, pages 118-120
Idiopathic Hemolytic Anemia of Pregnancy: A Diagnostic Dilemma
Monika Guptaa, b, Mansi Kalaa, Sanjay Kumara, Gajender Singha, Sonia Chhabraa, Rajeev Sena
aDepartment of Pathology, PGIMS, University of Health Sciences, Rohtak, India
bCorresponding Author: Monika Gupta, 17/8 FM, Medical Enclave, PGIMS, Rohtak, Haryana, India
Manuscript accepted for publication August 28, 2014
Short title: Idiopathic Hemolytic Anemia of Pregnancy
doi: http://dx.doi.org/10.14740/jh171w
| Abstract | ▴Top |
Hemolytic anemia is not uncommon in obstetric practice. However, a rare entity has been described, in which an idiopathic hemolytic anemia occurs during pregnancy, which gets resolved completely after delivery and recurs during subsequent pregnancy. We came across such a case in a young female in third trimester of her second pregnancy which was referred with complaints of severe anemia. On ultrasonographic examination the baby was normal for gestational age. Investigations performed revealed Coomb’s negative hemolytic anemia of unknown origin. She was treated with hematinics, blood transfusion and glucocorticoids. A healthy baby without evidence of hemolysis was delivered uneventfully through the vagina. The patient recovered during postpartum and was discharged with normal indices. As this condition is rare and exact cause is not known, also in our case first pregnancy was uneventful in contrast to the cases described in the literature, which merits its presentation.
Keywords: Hemolytic anemia; Coomb’s negative; Pregnancy
| Introduction | ▴Top |
Anemia in pregnancy has multi-factorial etiology. It is a common problem in most developing countries and a major cause of morbidity and mortality. Iron and folate deficiency anemias are common and related to nutritional deficiency and/or intestinal helminthic infections [1]. Pregnancy-induced hemolytic anemia is a rare maternal complication that occurs during pregnancy and resolves soon after delivery [2]. This is of unknown etiology, and the only factor clearly associated with the anemia is the gravid state. Characteristic of this problem is the absence of any identifiable immune mechanism or intracorpuscular/extracorpuscular defects despite the use of specific and sensitive complement-fixation techniques and assay of all red blood cell (RBC) enzymes [3]. We encountered a case of a 25-year-old female who developed severe life-threatening hemolytic anemia in the last trimester of her second pregnancy with spontaneous recovery after delivery.
| Case Report | ▴Top |
A 25-year-old female with 32 weeks of gestation presented with complaints of weakness, easy fatigability, difficulty in breathing and pallor. There was no history of bleeding or rupture of membranes, and fetal movements were perceived normally by her. She was on regular antenatal checkup and being quite well throughout the pregnancy until shortly before admission, when she felt sick and started having episodes of vomiting. She had no symptoms of infection during this pregnancy and only medications she was taking were oral iron and folic acid. Her previous pregnancy was uneventful 3 years ago. She had a normal vaginal delivery at home with no records available. There was no history of abortion. Family history was unremarkable for any bleeding disorder.
On examination she was pale and slightly icteric. Her body temperature was normal, pulse rate was 132/min and blood pressure was 120/60 mm Hg. There was a functional systolic ejection murmur at the apex. There was mild splenomegaly and liver was normal in size. The size of uterus corresponded to 32 weeks of gestation. Fetal heart rate was 130 beats/min.
Laboratory investigations revealed hemoglobin 6.0 g/dL, hematocrit 20%, mean cell volume 81.0 fL, mean cell hemoglobin 27.7 pg, mean corpuscular hemoglobin concentration 29.9 g/dL, total RBC count 4.0 × 109/µL and reticulocyte count 15%. Peripheral smear was normocytic moderately hypochromic with 25 normoblasts/100 WBCs seen. WBC count and platelet counts were also within normal limits. No hemoparasite was identified in the smear (Fig. 1).
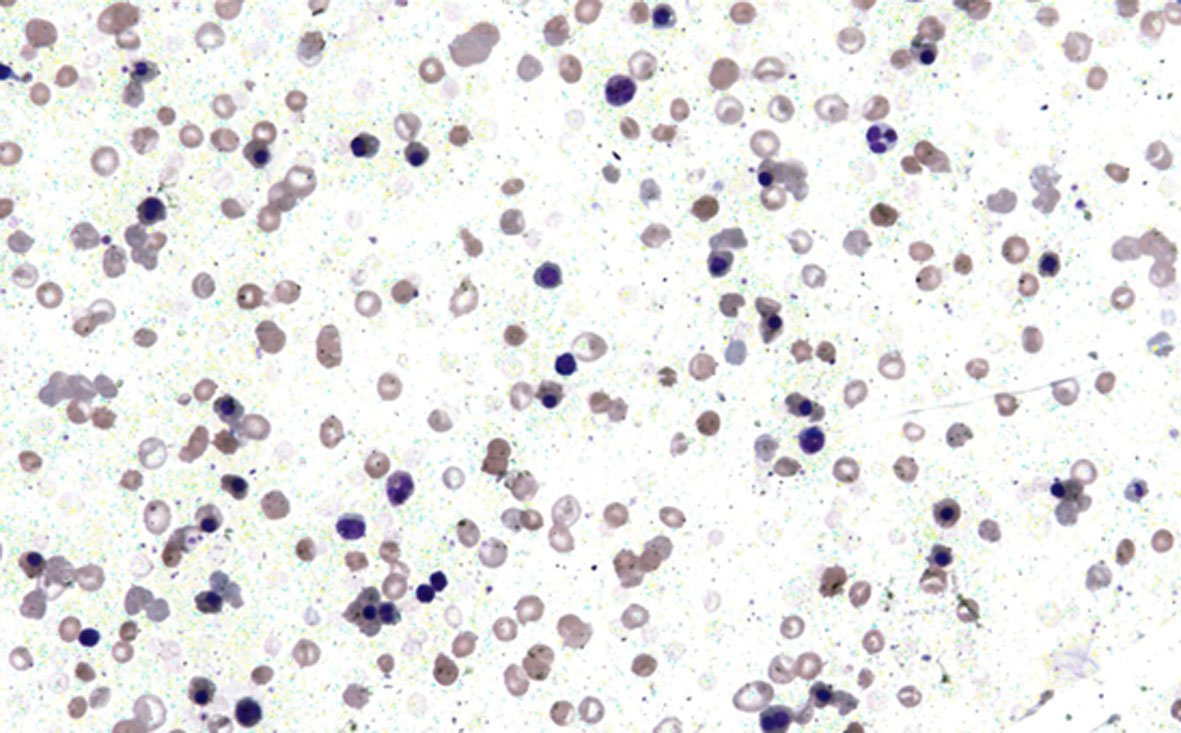 Figure 1. Peripheral blood smear showing normocytic moderately hypochromic RBCs along with nucleated RBCs and polychromatic cells (× 200). Figure 1. Peripheral blood smear showing normocytic moderately hypochromic RBCs along with nucleated RBCs and polychromatic cells (× 200). |
Liver function test revealed mild elevation of aspartate aminotransferase 68 IU and alanine aminotransferase 72 IU. Total bilirubin was 3.2 mg/dL with direct bilirubin of 0.8 mg/dL. On urine examination urobilinogen was strongly positive while hemoglobin and bilirubin were absent. Stool sample was negative for occult blood and parasites. Her blood group was “A” positive. The direct antiglobin test with specific anti-IgG anti-serum was negative.
On further workup, lactate dehydrogenase was raised to 460 mU/mL. Screening test for G6PD deficiency and osmotic fragility test were normal. Paroxysmal nocturnal hemoglobinuria (PNH) studies were noncontributory. Hemoglobin electrophoresis results were also within normal limits. The serum iron was 310 µg/dL with total iron binding capacity 356 µg/dL. The serum B12 and folic acid levels were normal. Normal values were obtained for other biochemical investigations like electrolytes, blood sugar, urea, creatinine and alkaline phosphatase. Negative results were also obtained on LE cell preparation and antinuclear antibodies.
Bone marrow examination revealed hypercellular marrow smears with reversed M:E ratio. Marrow showed normoblastic to micronormoblastic erythroid hyperplasia with adequate iron stores (Fig. 2). With the above investigations a diagnosis of Coomb’s negative hemolytic anemia of unknown cause was made.
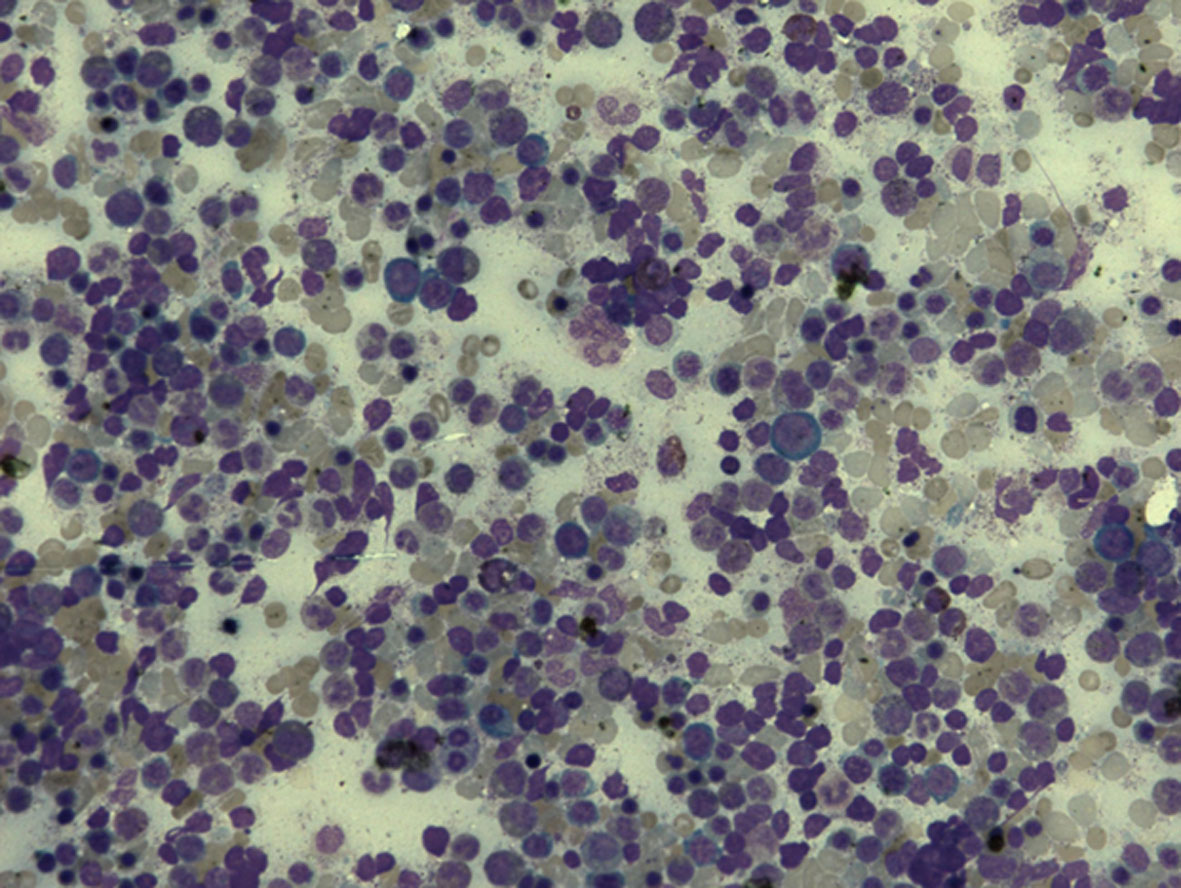 Figure 2. Bone marrow aspirate smear showing micronormoblastic to normoblastic erythroid hyperplasia along with myeloid cells in different stages of maturation (× 200). Figure 2. Bone marrow aspirate smear showing micronormoblastic to normoblastic erythroid hyperplasia along with myeloid cells in different stages of maturation (× 200). |
Patient was treated with folic acid and daily blood transfusion for 1 week but showed no improvement in her hematocrit. Decision was made to start glucocorticoids. Patient showed dramatic improvement with glucocorticoid, with improvement of blood picture (nRBC and polychromasia). At 37 weeks, she delivered a healthy male baby weighing 2.8 kg with no signs of hemolysis.
The patient was reevaluated 4 days after delivery and all her biochemical parameters returned to normal. The hemoglobin increased to 10.9 g%. Baby was fine, free of any signs and symptoms of hemolytic disease. After 1 week mother and baby were discharged. Patient did not turn up for follow-up.
| Discussion | ▴Top |
Anemia is one of the leading causes of maternal and perinatal deaths in pregnancy and puerperium. Hemolysis is one of the rare causes of severe anemia in pregnancy worldwide [4]. A rare entity called idiopathic hemolytic anemia has been described in pregnancy. The pathogenesis of this anemia is still not known; also the condition is not homogenous [5]. Literature search revealed few case reports with different pathogenesis and variation in the clinical manifestation. Cases reports showed that patient positive for IgG (warm antibodies, immune-mediated) responded well to glucocorticoids [5-7]. In contrast, majority of the cases were of non-immune mechanism, as was seen in our case.
So far, a few hypotheses have been proposed to explain the mechanism of destruction, one of which is malaria, which is negated in our case [4]. Splenomegaly in our patient may explain reduced RBC survival, but absence of splenectomy and improvement following steroids and delivery in our patient explain that this organ does not play an important part in the pathogenesis of this disease. Sometimes an immune hemolytic anemia occurs in few patients in whom concentration of antibody on the red cell is below the level for the detection by usual anti-globulin test. It is postulated that properties of antibody along with the sensitivity of reticuloendothelial system accounts for hemolytic anemia occurring at low concentration of antibody, and this mechanism might explain its response to glucocorticoids despite being Coomb’s negative [8].
Most of the cases usually present in the third trimester and improved with delivery and recurrence in subsequent pregnancies. However, in our case her first pregnancy was unremarkable. The anemia is usually severe, even life-threatening to the mother and fetus [9]. Whether pregnancy has any role to play in the etiology remains unclear; however, the fact that this patient improved at the end of her pregnancy cannot be denied. The mechanism of the increased red-cell destruction is obscure. The failure to demonstrate either auto-agglutinins or hemolysins in the circulating blood indicates that abnormal antibody formation is not a factor [10].
To embark on the diagnosis of idiopathic hemolytic anemia, it is essential to rule out other causes of non-immune hemolytic anemia, which include broad etiologies such as congenital, mechanical, toxic agents, medications, infection, PNH, lymphoproliferative disorder, etc. [3, 11, 12]. Extensive investigations were carried out to determine the cause of hemolysis in our case, but these proved unfruitful.
As Coomb’s negative hemolytic anemia is very rare in the population, management of such patient is challenging and controversial with scarce literature on this topic [3, 12]. Clinical observation is important in the management, as this patient responds to corticosteroid therapy, the mechanism being unclear. Multiple blood transfusion and iron supplements also play an important part in the management [4].
In our case the patient responded well to steroid, and her condition improved even more following the delivery of the baby. Preterm labor and low birth weight are among the reported complications of severe anemia in pregnancy [13]; however, in our case patient had a full term normal vaginal delivery of a healthy baby with normal hematological parameters.
Conclusion
Coomb’s negative hemolytic anemia of pregnancy, a rare entity, may be life-threatening, and needs tireless diagnostic and appropriate treatment approach for optimum maternal-fetal outcome. It responds to glucocorticoid therapy dramatically and its administration at the right time may improve fetal well-being. With early recognition and appropriate treatment the hazard of this condition can be avoided.
| References | ▴Top |
- Brabin BJ, Hakimi M, Pelletier D. An analysis of anemia and pregnancy-related maternal mortality. J Nutr. 2001;131(2S-2):604S-614S; discussion 614S-615S.
- Katsuragi S, Sameshima H, Omine M, Ikenoue T. Pregnancy-induced hemolytic anemia with a possible immune-related mechanism. Obstet Gynecol. 2008;111(2 Pt 2):528-529.
doi pubmed - Starksen NF, Bell WR, Kickler TS. Unexplained hemolytic anemia associated with pregnancy. Am J Obstet Gynecol. 1983;146(6):617-622.
pubmed - Dominico SA, Janmohamed M, Magesa A, Jaka H, Rambau PF, et al. Coombs Negative Hemolytic Anemia of Unknown Origin in Pregnancy. J Blood Lymph. 2012;2:103.
doi - Ng SC, Wong KK, Raman S, Bosco J. Autoimmune haemolytic anaemia in pregnancy: a case report. Eur J Obstet Gynecol Reprod Biol. 1990;37(1):83-85.
doi - Benraad CE, Scheerder HA, Overbeeke MA. Autoimmune haemolytic anaemia during pregnancy. Eur J Obstet Gynecol Reprod Biol. 1994;55(3):209-211.
doi - Baumann R, Rubin H. Autoimmune hemolytic anemia during pregnancy with hemolytic disease in the newborn. Blood. 1973;41(2):293-297.
pubmed - Gilliland BC. Coombs-negative immune hemolytic anemia. Semin Hematol. 1976;13(4):267-275.
pubmed - Hershko C, Berrebi A, Resnitzky P, Eldor A. Relapsing haemolytic anaemia of pregnancy with negative antiglobulin reaction. Scand J Haematol. 1976;16(2):135-140.
doi pubmed - Craig GA, Turner RL. A case of symptomatic haemolytic anaemia in pregnancy. Br Med J. 1955;1(4920):1003-1005.
doi - Sharma P and Sthapit R. Unexplained hemolytic anemia of pregnancy: Case report with review of related literature. NJOG. 2008;3:49-50.
- Kumar R, Advani AR, Sharan J, Barsharutallah MS, Al-Lumai AS. Pregnancy induced haemolytic anaemia; an unexplained entity. Ann Hematol. 2001;80:623-626.
doi pubmed - Kalaivani K. Prevalence & consequences of anaemia in pregnancy. Indian J Med Res. 2009;130(5):627-633.
pubmed
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Journal of Hematology is published by Elmer Press Inc.